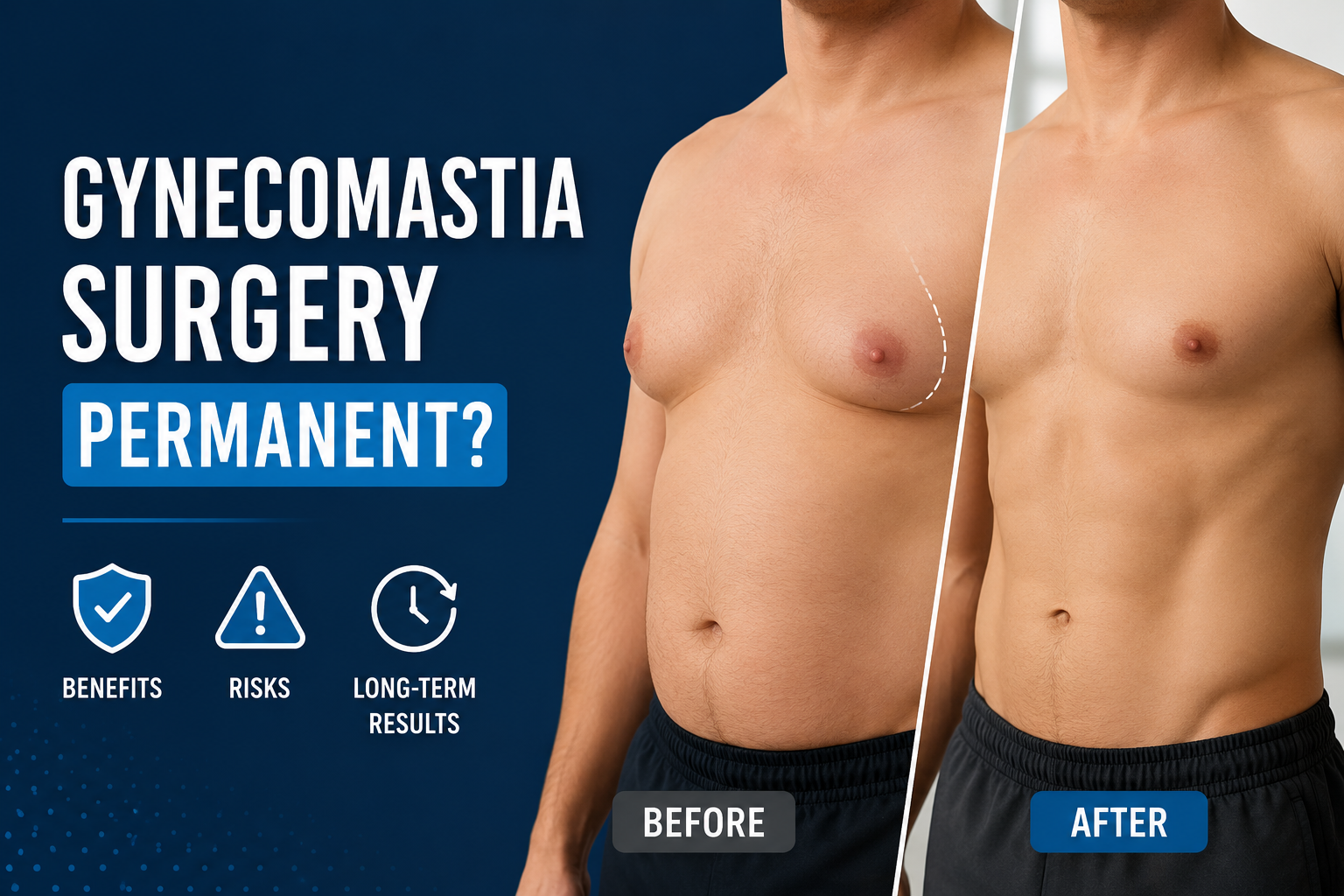
Gynecomastia is a medical condition characterized by the abnormal enlargement of glandular breast tissue in males, resulting in a protruding or feminized chest appearance. While it may seem like a purely cosmetic concern at first glance, gynecomastia carries a significant emotional and psychological burden for the men who live with it - affecting how they dress, how they move, how they interact socially, and how they perceive themselves. Many men with this condition avoid swimming pools, gyms, and intimate situations out of embarrassment, and some experience symptoms of anxiety and depression as a direct result.
Gynecomastia can affect one or both sides of the chest and can develop at virtually any age - from adolescence through adulthood and into old age. While the condition is more common than most people realize (affecting an estimated 40 to 60 percent of men to some degree), it is still widely misunderstood, underdiagnosed, and undertreated. Many men silently suffer for years before seeking professional help, often because they are unaware that effective, lasting solutions exist.
Surgery is widely regarded as the most reliable and effective treatment for gynecomastia, particularly in cases where the condition involves significant glandular tissue growth that will not respond to lifestyle changes or medication. Through the careful removal of excess glandular tissue and fatty deposits, gynecomastia surgery - also known as male breast reduction surgery - can restore a flatter, more masculine chest contour and, with it, a profound improvement in confidence and quality of life.
In this comprehensive guide, we cover everything you need to know about gynecomastia surgery: what causes the condition, who is a suitable candidate for surgery, how the procedure is performed, what results you can expect, how long recovery takes, and - most importantly - whether the results are permanent.
What Are the Causes of Gynecomastia?
Understanding the underlying cause of gynecomastia is a critical first step before pursuing any treatment option. The condition is not simply a result of being overweight - while excess fat can contribute to a puffy chest appearance (a condition sometimes called pseudogynecomastia), true gynecomastia specifically involves the growth of glandular breast tissue, which is driven by a range of hormonal, pharmacological, and physiological factors.
Hormonal Imbalance: The most common underlying cause of gynecomastia is an imbalance between the hormones estrogen and testosterone. All men naturally produce small amounts of estrogen, but when estrogen levels rise disproportionately relative to testosterone - or when testosterone levels fall - the breast tissue can be stimulated to grow. This hormonal shift is why gynecomastia frequently appears during puberty, when hormones are in flux, and again in older age, when testosterone production naturally declines.
Weight Gain: Excess body fat increases the body's conversion of androgens (male hormones) into estrogens, which can tip the hormonal balance toward estrogen dominance and stimulate breast tissue growth. Additionally, fat deposits in the chest area can add to the physical prominence of the condition, making the chest appear larger and more feminized.
Medications: A surprisingly wide range of prescription and over-the-counter medications are known to cause or contribute to gynecomastia as a side effect. These include certain antidepressants, anti-anxiety medications, blood pressure medications (particularly calcium channel blockers and spironolactone), ulcer medications, heart medications such as digoxin, and some antibiotics and antifungals. If you are taking any long-term medications and have developed gynecomastia, it is worth discussing this with your doctor.
Anabolic Steroid Use: The use of anabolic steroids - whether for athletic performance enhancement or bodybuilding - is a well-documented cause of gynecomastia. Anabolic steroids artificially elevate testosterone levels, which the body compensates for by converting excess androgens into estrogen, directly stimulating glandular tissue growth in the chest.
Genetics: Some men have a hereditary predisposition to developing gynecomastia, regardless of their weight, hormonal health, or lifestyle. If the condition runs in your family, you may be more likely to develop it even without other contributing factors.
Underlying Health Conditions: Certain medical conditions can contribute to gynecomastia, including liver disease (which affects hormone metabolism), kidney failure, thyroid disorders, and tumors affecting the pituitary gland or adrenal glands. These should always be ruled out before attributing gynecomastia to lifestyle or hormonal causes alone.
In some cases - particularly in adolescents - gynecomastia resolves on its own as hormone levels naturally stabilize. However, when glandular tissue has firmly established itself and the condition has persisted for more than a year or two, spontaneous resolution becomes unlikely, and surgical intervention is typically the most reliable path to correction.
What Is Gynecomastia Surgery?
Gynecomastia surgery, clinically referred to as reduction mammaplasty or male breast reduction surgery, is a surgical procedure specifically designed to address the physical manifestations of gynecomastia by removing the excess glandular tissue, fat, and in some cases skin that has accumulated in the chest area. The goal is to create a chest contour that is flatter, firmer, and more consistent with a traditionally masculine appearance.
The specific surgical approach used depends on the composition of the enlarged chest tissue and the severity of the condition. In cases where the enlargement is primarily due to excess fatty tissue with minimal glandular involvement, liposuction alone may be sufficient to achieve the desired result. Liposuction involves making small incisions through which a thin cannula (tube) is inserted to break up and suction out the fatty deposits. This approach leaves minimal scarring and offers a relatively straightforward recovery.
When the enlargement involves significant glandular tissue - which is firmer and more fibrous than fat and cannot be effectively removed by liposuction - excisional surgery is required. This involves making a small incision, typically along the edge of the areola (the pigmented skin surrounding the nipple) where it naturally blends with the surrounding skin, through which the glandular tissue is carefully excised. This incision placement is deliberate - it allows the surgeon to access and remove the tissue while keeping the resulting scar as inconspicuous as possible.
In many cases, a combination of both liposuction and excision is used to address mixed-composition gynecomastia, remove both fatty and glandular components, and achieve the most refined and natural-looking chest contour possible. In more severe cases - particularly those involving significant skin laxity or excess skin resulting from major weight loss or extreme tissue enlargement - additional skin removal and repositioning may also be necessary.
The procedure is performed under general anesthesia or, in some cases, local anesthesia with sedation, depending on the extent of surgery and the patient's and surgeon's preferences. It typically takes between one and two hours to complete from start to finish.
Who Is a Suitable Candidate for Male Breast Reduction?
Gynecomastia surgery is appropriate for a broad range of men, but not every man with gynecomastia is an ideal candidate at every point in time. Determining candidacy involves a careful evaluation of multiple factors - physical, medical, and psychological - to ensure that surgery is both safe and likely to produce the outcomes the patient is hoping for.
In general, you may be a good candidate for gynecomastia surgery if you have persistent chest fullness or breast tissue enlargement that has not responded to lifestyle changes, weight loss, or medication adjustments. Suitable candidates are men who feel self-conscious, uncomfortable, or psychologically distressed by the appearance of their chest and who have realistic, well-informed expectations about what surgery can achieve.
Physical health is a prerequisite - candidates should be in good general health without untreated medical conditions that would significantly elevate surgical risk. Non-smokers or those who are willing to stop smoking well in advance of surgery are preferred, as smoking impairs wound healing and increases complication risks. Candidates should also be at or near a stable, healthy body weight, as significant weight fluctuation after surgery can compromise results.
It is also important that the gynecomastia itself has stabilized before surgery is considered. This is particularly relevant for teenagers and young men - if hormones are still fluctuating and the condition has not yet reached its final state, operating too early risks the tissue regrowing after surgery. Most specialists recommend waiting until the mid-to-late teenage years at the earliest, and only if the condition has been stable for at least one to two years.
Finally, if an underlying cause of gynecomastia - such as a medication, substance, or medical condition - has been identified, this should ideally be addressed before or alongside surgery. In some cases, treating the root cause may reduce the severity of the condition or prevent recurrence after surgery.
Is Gynecomastia Surgery Permanent?
This is the question that weighs most heavily on the minds of men considering surgery - and the good news is that, in the vast majority of cases, gynecomastia surgery does produce permanent results. Understanding why this is the case, and under what circumstances results might not be permanent, requires a brief explanation of what the surgery actually removes.
Why Results Are Generally Permanent: The primary reason gynecomastia surgery produces lasting results is that surgeons physically remove the glandular tissue from the chest. Unlike fat cells, which can enlarge with weight gain, true glandular breast tissue does not regenerate or regrow once it has been surgically excised. The cells are gone permanently. In cases where liposuction is used to remove fatty tissue, the number of fat cells in the treated area is permanently reduced, significantly decreasing the capacity for fat to re-accumulate in that specific location. Together, these factors mean that the vast majority of men who undergo gynecomastia surgery enjoy a flat, masculine chest contour for the rest of their lives.
Factors That Can Affect Long-Term Results: While the surgery itself produces permanent tissue removal, the long-term appearance of the chest can still be influenced by lifestyle and health factors. Significant weight gain after surgery can cause the remaining fat cells in the chest area to enlarge, potentially recreating some degree of fullness. Hormonal imbalances - whether due to aging, medical conditions, or the use of substances such as anabolic steroids - can theoretically stimulate any residual glandular tissue to grow. Certain medications taken after surgery may also have gynecomastia as a side effect.
In summary, gynecomastia surgery is as close to permanent as any cosmetic surgical procedure can be - provided that the patient maintains a stable body weight, avoids substances known to cause hormonal disruption, and addresses any underlying hormonal conditions. For most men, surgery represents a definitive, lifelong solution to a condition that has often caused years of distress.
How Does the Procedure Go?
The gynecomastia surgery process begins well before the day of the operation itself. A thorough preoperative evaluation is an essential part of ensuring that the procedure is safe, appropriately planned, and set up for the best possible outcome.
Consultation and Preoperative Evaluation: Your journey begins with a detailed consultation with your surgeon. During this appointment, the surgeon will assess the composition and severity of your gynecomastia, evaluate the quality and elasticity of your chest skin, discuss your medical history and any medications you are taking, and listen carefully to your aesthetic goals and concerns. Preoperative tests - including blood work, a physical examination, and sometimes imaging - may be ordered to ensure you are fit for surgery and to rule out any underlying conditions contributing to the gynecomastia.
Anesthesia: On the day of surgery, anesthesia is administered before the procedure begins. Most gynecomastia surgeries are performed under general anesthesia, meaning you will be completely asleep and pain-free throughout the procedure. In some cases, local anesthesia combined with sedation may be appropriate for less extensive procedures.
Tissue Removal: Depending on your specific case, the surgeon will proceed with liposuction, excision, or a combination of both. Liposuction involves small incisions through which a thin cannula is inserted to suction out fatty tissue. Excision involves carefully removing glandular tissue through a precisely placed incision, typically at the lower border of the areola. The surgeon works methodically and precisely to remove the appropriate amount of tissue while preserving the natural contour and symmetry of the chest.
Chest Contouring: Once the excess tissue has been removed, the surgeon carefully sculpts and refines the chest contour to ensure a natural, masculine shape. Attention is paid to symmetry, nipple positioning, and the overall proportions of the chest relative to the patient's body.
Incision Closure: The small incisions are sutured closed using fine sutures, and dressings are applied. A compression garment is fitted immediately after the procedure to support the healing tissues, minimize swelling, and help the skin conform smoothly to its new contours.
The entire procedure typically takes between one and two hours, after which the patient is moved to a recovery area and monitored as the anesthesia wears off. Most patients are discharged the same day.
Advantages of Gynecomastia Surgery
The benefits of gynecomastia surgery extend far beyond the purely physical - while the visible changes to the chest are often dramatic and immediately life-changing, the deeper, longer-lasting benefits are frequently psychological and emotional in nature.
A Flatter, More Masculine Chest Contour: The most obvious and immediate benefit is the physical transformation of the chest. Surgery removes the excess tissue that creates the feminized appearance and replaces it with a flat, toned, masculine contour. For many men, this is a result that no amount of diet or exercise could have achieved, because glandular tissue - unlike fat - does not respond to caloric deficit or strength training.
Improved Body Proportions: Gynecomastia can distort the overall proportions of the upper body, making even a lean and muscular physique look unbalanced. By flattening the chest and restoring natural contours, surgery improves the overall visual harmony of the body, making the shoulders appear broader and the torso more defined.
Freedom in Clothing Choices: Many men with gynecomastia spend years carefully selecting and layering clothing to disguise their chest, avoiding fitted shirts, light-colored fabrics, and situations where they might be seen without a shirt. After surgery, this burden is lifted entirely - patients can wear whatever they choose with comfort and confidence.
Enhanced Confidence and Self-Esteem: The psychological impact of gynecomastia surgery is frequently described by patients as one of the most transformative aspects of the procedure. Men who have spent years feeling ashamed of or embarrassed by their bodies often report a dramatic improvement in self-esteem, social confidence, and overall mental well-being following surgery.
Improved Quality of Life: Beyond aesthetics and confidence, surgery allows men to participate more freely in physical activities - including swimming, sports, and gym workouts - that they may have previously avoided out of self-consciousness. This improved engagement with physical activity further supports long-term health and well-being.
How Do Gynecomastia Surgery Results Look?
The primary aesthetic goal of gynecomastia surgery is to create a chest that looks natural, masculine, and proportional - not a chest that looks operated on. When performed by a skilled and experienced surgeon, the results are typically subtle enough that most observers would not be able to tell that a procedure had been done, yet significant enough to dramatically change the patient's appearance and self-perception.
After complete healing and recovery, patients can expect the chest contour to be noticeably flatter and firmer. The overall body contour becomes more defined and balanced, particularly in the upper body. The nipples and areolas, which may have protruded or appeared enlarged prior to surgery, typically settle into a more natural, flatter position that aligns harmoniously with the surrounding chest. Excess skin, if present, contracts and tightens over time as healing progresses.
It is important to note that final results are not immediately visible - the healing process unfolds gradually over several months. In the early postoperative period, swelling obscures the true outcome of surgery. As swelling resolves week by week, the chest contour becomes progressively clearer and more refined. Most surgeons consider the results to be fully visible and settled approximately three to six months after surgery, although some degree of subtle ongoing improvement can continue for up to a year.
The quality of the final result is influenced by several factors, including the severity and composition of the preoperative gynecomastia, the elasticity and quality of the patient's skin, the surgical technique employed, and the patient's adherence to postoperative care instructions. Patients with good skin elasticity tend to achieve the smoothest, most natural-looking results, while those with significant skin laxity may require additional procedures to address excess skin.
Immediate Post-Surgical Changes
The first 24 to 72 hours following gynecomastia surgery are a time of active healing, and patients should be prepared for a period of discomfort and physical limitation during this phase. Understanding what to expect in the immediate postoperative period helps patients manage their recovery effectively and avoid unnecessary anxiety about normal symptoms.
In the first few days after surgery, patients commonly experience moderate to significant swelling in the chest area. This swelling is a normal and expected part of the healing response and is not cause for alarm. The chest may also feel tight, heavy, and sensitive to the touch. Bruising is common and may spread across the chest and upper abdomen before gradually fading over the following one to two weeks.
Physical movement is restricted in the immediate postoperative period, particularly movements that involve the arms, shoulders, and upper body. Patients are advised to move slowly and carefully, avoid reaching overhead or lifting anything heavier than a cup of water, and sleep in an elevated position to help minimize swelling. Pain is typically well-managed with prescribed oral pain medications and anti-inflammatory drugs.
A compression garment is one of the most important tools in the early recovery period. This fitted elastic garment is worn continuously - day and night - for the first several weeks after surgery. It serves multiple purposes: reducing swelling by providing consistent gentle pressure to the healing tissues, supporting the chest as the skin conforms to its new contours, and helping to minimize the risk of fluid accumulation (seroma) beneath the skin.
Setting Realistic Expectations
One of the most important conversations a patient can have with their surgeon before gynecomastia surgery is an honest discussion about realistic expectations. While the procedure can produce genuinely remarkable improvements, it is essential that patients approach surgery with accurate, grounded expectations rather than idealized notions of a perfect outcome.
It is important to understand that no surgical procedure can guarantee a perfectly flat chest in absolute terms - the chest will always retain some natural, slight degree of volume and contour, reflecting the underlying anatomy. What surgery can do is dramatically reduce the excess tissue and create a chest that appears flat, natural, and masculine in proportion to the patient's body.
Swelling will be present for weeks to months after surgery, and this swelling temporarily distorts the visible results. Patients should resist the urge to judge their final outcome too early in the recovery process. The true, settled results of surgery will only be fully apparent once all swelling has resolved, which typically takes three to six months.
Scarring is also a realistic expectation - any surgical procedure that involves incisions will leave some degree of scarring. In gynecomastia surgery, incisions are carefully placed to be as inconspicuous as possible, and scars typically fade significantly over time. However, patients with a tendency toward thick or raised scarring (hypertrophic scars or keloids) should discuss this with their surgeon during the consultation, as it may influence the approach taken.
A thoughtful, experienced surgeon will walk patients through all of these nuances during the preoperative consultation, ensuring that everyone proceeds with a clear, realistic understanding of what the surgery can - and cannot - deliver.
Gynecomastia Recovery: Stages and Timeline
Recovery from gynecomastia surgery follows a predictable progression through several distinct stages, each marked by improving comfort, decreasing swelling, and an increasingly clear view of the final results. Understanding this timeline in advance helps patients manage their expectations, plan their work and social commitments accordingly, and recognize which symptoms are normal versus which warrant a call to the clinic.
Days 1–3: Immediate Post-Surgery Phase
The first two to three days after surgery are typically the most uncomfortable. Moderate to strong discomfort, significant chest swelling, bruising, tightness, and restricted movement of the upper body are all normal and expected during this phase. Pain medications prescribed by your surgeon will help manage discomfort effectively. Rest is the priority - patients should remain at home, move carefully and minimally, and avoid any activities that strain the upper body. The compression garment must be worn continuously during this period.
Week 1: Early Recovery
By the end of the first week, most patients notice that their discomfort has begun to decrease meaningfully and that they are able to move more comfortably. Swelling remains present but may begin to slowly reduce. Bruising is typically most visible during this week before it begins to fade. Most patients are able to perform very light daily activities - such as short walks around the house - but should continue to avoid anything strenuous. The compression garment continues to be worn at all times. A follow-up appointment with the surgeon is typically scheduled during the first week to assess healing and remove any drains if they were placed.
Weeks 2–3: Improving Comfort and Mobility
During the second and third weeks after surgery, patients typically experience a significant improvement in comfort and a noticeable reduction in swelling. Bruising fades considerably or disappears entirely. The chest contour begins to look clearer, and many patients get their first encouraging glimpse of what their final result will look like. Most men are able to return to desk-based or sedentary work during this period, and light, non-strenuous daily activities can be resumed. The compression garment continues to be worn, though some surgeons may begin to allow brief periods without it.
Weeks 4–6: Resumed Activity and Continued Healing
By four to six weeks post-surgery, most patients feel nearly back to normal in terms of daily comfort. Swelling continues to diminish, and only minor residual swelling may remain. Light exercise - such as walking, gentle cycling, or lower-body workouts that do not engage the chest - can typically be resumed during this period, with your surgeon's approval. The chest contour becomes increasingly defined and stable as healing progresses.
2–3 Months: Final Results Emerge
Complete healing and the full revelation of final surgical results typically occur between two and three months after surgery. By this point, swelling has resolved entirely, the skin has conformed smoothly to the new chest contour, and any minor residual changes from the healing process have settled. Patients can resume all forms of exercise, including chest-focused strength training, with their surgeon's clearance. The chest appears flat, firm, and natural - the result that patients have been waiting for throughout the recovery process.
Gynecomastia Recovery: Essential Care Tips
Following your surgeon's postoperative care instructions diligently is one of the most important things you can do to support your healing, minimize complications, and optimize your final results. Recovery from gynecomastia surgery is not passive - active participation in your own care makes a meaningful difference in how smoothly and successfully the process unfolds.
Wear Your Compression Garment Consistently: The compression garment is not optional - it is a critical component of recovery. Wear it exactly as directed by your surgeon, typically around the clock for the first several weeks. It helps reduce swelling, prevents fluid accumulation, and supports the chest tissues as they heal and contract to their new contours.
Protect Your Incisions: Keep incision sites clean and dry as directed, and avoid submerging them in water (baths, swimming pools, or the ocean) until your surgeon confirms they have fully healed. Protect healing scars from sun exposure, as UV rays can permanently darken scar tissue. Once healing is complete, scar massage and silicone-based scar treatments can help minimize the appearance of residual scarring.
Avoid Physical Strain: Refrain from any activity that strains the upper body, engages the chest muscles, or significantly elevates your heart rate during the early recovery weeks. This includes heavy lifting, reaching overhead, vigorous cardiovascular exercise, and contact sports. Returning to exercise too soon increases the risk of swelling, bleeding, and delayed healing.
Maintain a Nutritious Diet and Stay Hydrated: Good nutrition supports tissue repair and immune function during the healing process. Focus on a balanced diet rich in protein, vitamins, and minerals, and drink plenty of water. Avoid alcohol and smoking throughout the recovery period, as both impair circulation and wound healing.
Attend All Follow-Up Appointments: Regular check-ins with your surgeon throughout the recovery period are essential. These appointments allow your surgeon to monitor your healing, identify and address any early signs of complications, and provide guidance on when it is safe to resume various activities. Never skip follow-up appointments, and always contact the clinic promptly if you notice anything unusual or concerning.
Possible Risks and Complications
Like all surgical procedures, gynecomastia surgery carries some degree of risk, and it is important that patients are fully informed about potential complications before making a decision to proceed. The overall complication rate for gynecomastia surgery performed by experienced, board-certified surgeons is low, but being aware of what can go wrong allows patients to make truly informed decisions and to recognize early warning signs during recovery.
Common minor and expected side effects include swelling, bruising, temporary numbness or altered sensation in the chest and nipple area, and discomfort at the incision sites. These are entirely normal aspects of the healing process and resolve on their own over the course of recovery.
More significant complications are less common but possible. Infection at the surgical site can occur and may require antibiotic treatment or, in rare cases, additional intervention. Seroma - the accumulation of fluid beneath the skin - can develop and may need to be drained by the surgeon. Hematoma (collection of blood beneath the skin) is another possible complication that, if significant, may require drainage.
In a small number of cases, patients may experience contour irregularities, such as asymmetry between the two sides of the chest, or subtle surface irregularities in the skin. These may improve with time and further healing, or may require minor revision procedures. Scarring, while inevitable to some degree with any incision-based surgery, is usually minimal and well-concealed, though individuals who are prone to hypertrophic or keloidal scarring may experience more noticeable scars.
Choosing a highly qualified and experienced surgeon, following all preoperative and postoperative instructions carefully, attending all follow-up appointments, and being honest with your surgical team about your medical history and any concerns that arise during recovery are all critical strategies for minimizing risk and ensuring the safest possible outcome.
Can Gynecomastia Come Back After Surgery?
One of the most reassuring aspects of gynecomastia surgery is that, in the overwhelming majority of cases, the condition does not return after surgery. Because the glandular tissue responsible for the condition is physically removed during the procedure, it cannot simply regrow on its own. Similarly, the fat cells removed through liposuction do not regenerate. For most men, surgery represents a definitive, permanent resolution of a condition they may have struggled with for many years.
That said, there are specific circumstances under which some degree of recurrence is possible, and understanding these allows patients to make informed lifestyle choices that protect their long-term results.
Significant weight gain after surgery is one of the most common reasons for a perceived recurrence. While the removed fat cells do not return, the remaining fat cells in the chest area can enlarge with weight gain, potentially recreating some degree of chest fullness. This is why maintaining a stable, healthy body weight after surgery is so important for preserving results.
Hormonal disruptions - whether caused by aging, an underlying medical condition, or the use of anabolic steroids or certain medications - can theoretically stimulate any small amounts of residual glandular tissue to proliferate. Men who use anabolic steroids after surgery are at a particularly elevated risk of recurrence and are strongly advised to discontinue their use permanently.
If you are taking a medication that contributed to your gynecomastia, discuss this with both your prescribing physician and your surgeon before and after surgery. Switching to an alternative medication where possible may be an important part of protecting your surgical results long term.
Factors Influencing the Effectiveness of Gynecomastia Surgery Results
The long-term success of gynecomastia surgery is not determined by the procedure alone - it is shaped by a complex interplay of surgical, biological, and lifestyle factors that together determine how well and how durably the results hold over time.
Surgical Technique and Surgeon Experience: The skill, experience, and aesthetic sensibility of the operating surgeon are among the most significant determinants of outcome quality. An experienced gynecomastia surgeon will choose the most appropriate technique for each patient's unique anatomy, remove the right amount of tissue to achieve a natural result without overcorrection, and minimize the risk of complications through precise, careful technique. Choosing a board-certified plastic surgeon with specific expertise in gynecomastia surgery is one of the most important decisions a patient can make.
Skin Quality and Elasticity: The quality and elasticity of the patient's skin significantly influences the final aesthetic result, particularly in terms of how smoothly and tightly the skin conforms to the new chest contour after tissue removal. Younger patients with good skin elasticity typically achieve the smoothest, most refined results. Patients with reduced skin elasticity - due to aging, significant weight loss, or other factors - may experience some degree of skin laxity after surgery, which may require additional treatment.
Lifestyle Habits: Long-term results are best preserved by maintaining a healthy, stable lifestyle after surgery. This includes maintaining a healthy body weight through diet and regular exercise, avoiding anabolic steroids and substances known to disrupt hormonal balance, limiting alcohol consumption, and not smoking. These habits support not only the preservation of surgical results but overall health and well-being.
Hormonal Health: Because hormonal imbalance is one of the most common underlying causes of gynecomastia, addressing and managing hormonal health is an important part of protecting long-term results. This may involve working with an endocrinologist if a specific hormonal disorder has been identified, and having periodic hormonal evaluations to detect and address any changes early.
Gynecomastia Surgery: Emotional Impact
While the physical transformation achieved through gynecomastia surgery is often remarkable, the emotional and psychological impact of the procedure is, for many patients, the most profound and meaningful change of all. Men who have spent years - sometimes decades - feeling ashamed of, embarrassed by, or limited by their chest frequently describe the experience of recovery as genuinely life-changing in ways that go far beyond appearance.
The psychological burden of gynecomastia is widely underestimated by those who have not experienced it firsthand. Many men with the condition develop deeply ingrained habits of avoidance and concealment - choosing clothing specifically to hide their chest, declining invitations to beach or pool events, avoiding the gym out of fear of judgment, and feeling profoundly uncomfortable in intimate situations. These avoidance behaviors can gradually restrict a man's life in meaningful ways, limiting social connection, physical activity, and self-expression.
After surgery and recovery, patients commonly report feeling as though a long-standing weight has been lifted. The freedom to wear a fitted T-shirt without anxiety, to take off their shirt at the pool without self-consciousness, to look in the mirror with pride rather than shame - these are experiences that many post-surgical patients describe as transformative. Studies on the psychological outcomes of gynecomastia surgery consistently show significant improvements in self-esteem, body image satisfaction, and overall quality of life.
It is also common for patients to notice improvements in their social confidence, interpersonal relationships, and willingness to engage in physical activity - all of which have ripple effects across every domain of their lives. For many men, gynecomastia surgery is not just a cosmetic procedure. It is a restoration of confidence, comfort, and freedom that they had resigned themselves to never having.
When Can I Return to Normal Life?
One of the most practical questions patients ask in the lead-up to surgery is when they can expect to return to their normal daily routines - work, exercise, social activities, and sports. While every patient's recovery is unique and the specific timeline should always be confirmed with your surgeon, the following general milestones provide a useful framework for planning.
Most patients are able to resume light, sedentary work - such as desk-based or computer work - within one to two weeks of surgery, provided their job does not involve physical labor, heavy lifting, or significant upper body activity. Men whose work involves manual labor, physical exertion, or frequent use of the arms and shoulders will typically need to take a longer period of leave - usually four to six weeks - before returning to full work duties.
Light physical activity, such as gentle walking, can typically be resumed within the first two weeks and is in fact encouraged as it promotes healthy circulation and speeds recovery. More significant cardiovascular exercise - jogging, cycling, swimming - can usually be reintroduced gradually from around the four to six week mark, subject to your surgeon's assessment. Full return to upper body strength training and contact sports is typically cleared at around six weeks post-surgery, once healing is sufficiently advanced to tolerate the additional physical stress.
Social activities and daily life routines outside of physical demands can generally resume within the first one to two weeks for most patients, though wearing the compression garment may affect some clothing choices during the initial recovery period. By the six-week mark, the vast majority of patients feel fully returned to their normal daily life and are enjoying the early benefits of their surgical results.
Conclusion
Gynecomastia surgery offers a highly effective and long-lasting solution for men struggling with enlarged breast tissue and the emotional challenges that often accompany it. By removing excess glandular tissue and fat, the procedure restores a flatter, more masculine chest contour that cannot typically be achieved through diet or exercise alone. For most patients, the results are not only physically transformative but also deeply empowering on a psychological level.
One of the most reassuring aspects of this procedure is its permanence. Since the glandular tissue is surgically removed, it does not regenerate. However, maintaining results depends on lifestyle choices such as stable weight management, avoiding anabolic steroids, and addressing any hormonal imbalances. When these factors are controlled, the outcomes of gynecomastia surgery can last a lifetime.
It is equally important to approach the procedure with realistic expectations and to choose a qualified, experienced surgeon who understands both the technical and aesthetic aspects of male chest contouring. With proper planning, adherence to post-operative care, and a commitment to long-term health, gynecomastia surgery can significantly enhance confidence, comfort, and overall quality of life—allowing individuals to move forward without the limitations they once faced.
Frequently Asked Questions (FAQs):-
Q: Is gynecomastia surgery a definitive solution for male breast enlargement?
A: Yes, in the vast majority of cases, gynecomastia surgery is a permanent solution. Surgeons physically remove the glandular tissue, which does not regenerate after excision. As long as patients maintain a stable weight, avoid anabolic steroids, and manage hormonal health, the results are typically long-lasting and life-changing.
Q: Will the symptoms of gynecomastia recur after surgery?
A: Recurrence is uncommon but possible under certain conditions. Significant weight gain, hormonal imbalances, anabolic steroid use, or specific medications can trigger some regrowth or chest fullness after surgery. Maintaining a healthy lifestyle and stable hormonal health is the most effective way to prevent recurrence and protect your results long term.
Q: What risks and complications can I face after surgery?
A: Potential complications include swelling, bruising, temporary numbness, infection, seroma (fluid accumulation), hematoma, contour irregularities, and scarring. Serious complications are uncommon when surgery is performed by a qualified, experienced surgeon. Following all preoperative and postoperative instructions significantly reduces your individual risk of complications.
Q: How much time does it take to recover from gynecomastia surgery?
A: Most patients return to light daily activities within one to two weeks and to desk work shortly after. Strenuous activity and upper body exercise are cleared at around four to six weeks. Final results, with all swelling fully resolved, are typically visible two to three months after surgery.
Q: What factors influence the efficiency of gynecomastia surgery results?
A: Key factors include the surgeon's technique and experience, the patient's skin quality and elasticity, overall lifestyle habits (weight management, avoidance of steroids), and hormonal health. Patients who maintain a stable, healthy lifestyle and follow all postoperative instructions consistently achieve the best and most durable long-term results.
Q: At what age is gynecomastia surgery most appropriate?
A: Most specialists recommend waiting until the mid-to-late teenage years at the earliest, and only when the condition has been stable for at least one to two years. For adults, there is no upper age limit - suitability is determined by overall health, the severity of gynecomastia, and the patient's skin quality rather than age alone.
Q: Will gynecomastia surgery leave visible scars?
A: Scarring is a normal outcome of any incision-based surgery, but gynecomastia incisions are deliberately placed along the natural border of the areola to minimize visibility. For most patients, scars fade significantly over six to twelve months. Scar massage and topical silicone treatments can further reduce their appearance during the healing process.
Q: How do I choose the right surgeon for gynecomastia surgery?
A: Choose a board-certified plastic surgeon with specific experience and a strong portfolio of gynecomastia cases. Review before-and-after photographs, read patient reviews, and ensure that your surgeon listens carefully to your concerns during the consultation. Never choose a surgeon based on price alone - expertise and artistry are what determine the quality of your outcome.
Q: Can exercise alone resolve gynecomastia without surgery?
A: No - true gynecomastia involves glandular tissue, which does not respond to diet or exercise. While losing weight through exercise may reduce associated fatty tissue and improve the overall appearance of the chest, the glandular component can only be removed surgically. If your chest fullness persists despite being at a healthy weight, surgery is likely the appropriate solution.
Q: Is gynecomastia surgery covered by insurance?
A: Coverage varies significantly depending on your insurance provider and the specific policy. In cases where gynecomastia is causing documented physical symptoms - such as pain, tenderness, or discomfort - or is linked to an underlying medical condition, some degree of coverage may be possible. Purely cosmetic procedures are generally not covered. It is advisable to consult your insurance provider directly and to obtain a letter from your physician documenting the medical necessity of the procedure if applicable.

